HPV vaccine hailed life-saving as cervical cancer rates drop - who can get it?
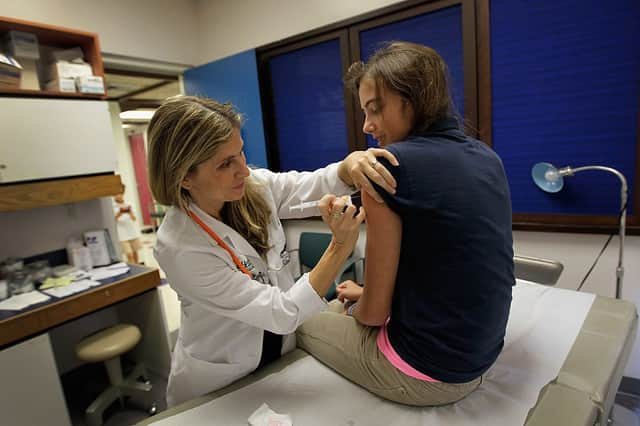

The NHS rollout of the HPV vaccine has helped prevent hundreds of women from developing cervical cancer and stopped thousands from experiencing pre-cancerous changes to cells, a new study has found.
The Cancer Research UK-funded research found that cervical cancer rates among women who were offered the vaccine between ages 12 and 13, and are now in their 20s, were 87% lower than in an unvaccinated population.
Advertisement
Hide AdAdvertisement
Hide AdCases in this age group, which are rare, also dropped from around 50 per year to just five.
Researchers also found a 62% reduction in cervical cancer rates in women who were vaccinated between 14 and 16, and 34% in women aged 16 to 18.
Experts assessed data from the human papillomavirus (HPV) immunisation programme using the vaccine Cervarix, which was given to girls on the NHS from 2008 to September 2012.
A different vaccine, Gardasil, is now used for the programme and is given to both girls and boys aged 12 and 13.
Advertisement
Hide AdAdvertisement
Hide AdThe findings, published in The Lancet medical journal, provide the first direct worldwide evidence of prevention of cervical cancer using a vaccine for two types of HPV.
What is HPV?
HPV, or human papillomavirus, is the name given to a common group of viruses.
There are more than 100 different types of HPV which typically affect the mouth, throat or genital area.
Some types are “high risk” as they are linked to the development of cancer, including cervical, vaginal and anal cancer, while other types can cause common conditions such as warts or verrucas.
Advertisement
Hide AdAdvertisement
Hide AdHPV is very common and can be caught through any kind of sexual contact with someone who already has it.
It affects most people at some stage in their life, although for many, their body will get rid of it without the need for treatment.
However, those who are infected with a high-risk type will not be able to clear it naturally.
These types can cause abnormal tissue growth and other changes which can lead to cancer if left untreated.
Who can get vaccinated against HPV?
Advertisement
Hide AdAdvertisement
Hide AdThe HPV vaccine is offered to girls and boys aged 12 and 13 years old (born after 1 September 2006) as part of the NHS vaccination programme.
In England, girls and boys in this age group are routinely offered their first vaccine in school Year 8, with the second dose given between six and 24 months afterwards.
Those who are eligible to get vaccinated and missed getting their first dose in Year 8 can still get it for free on the NHS up until their 25th birthday.
If you had your first dose at age 15 or above, you will need to have three doses of the vaccine as the body does not respond as well to two doses in older age groups.
Why are boys given the vaccine?
Advertisement
Hide AdAdvertisement
Hide AdThe vaccination programme was extended to boys aged 12 and 13 in England in July 2018 following advice from the Joint Committee on Vaccination and Immunisation (JCVI).
This decision was made to help prevent boys, as well as girls, from getting HPV-related cancers, including head, neck, anal and genital cancers.
Older boys who missed out on the offer of a vaccine do not need to get a jab as evidence suggests that they have already built up indirect protections, or herd immunity, over the 10 years the girls’ vaccine rollout has been running.
How does the vaccine work?
Since 2012, Gardasil has been the HPV vaccine given on the NHS vaccination programme.
Advertisement
Hide AdAdvertisement
Hide AdAt some point during the 2021 to 2022 academic year, this will switch to Gardasil 9 which protects against nine different types of HPV, including 6, 11, 16, 18, 31, 33, 45, 52 and 58.
Of these, types 16 and 18 are the cause of the most cervical cancers in the UK, accounting for more than 80%.
Types 31, 33, 45, 52 and 58 cause an additional 15% of cervical cancers, while types 6 and 11 cause around 90% of genital warts, so using this vaccine will help to protect both girls and boys against cancer and genital warts.